Many people experience shoulder pain at some point in their lives. This discomfort can arise from various causes, ranging from muscle strains to more complex joint issues. A question that commonly arises for those experiencing pain is, “Can you get arthritis in your shoulder?” The answer is yes, and understanding this condition is an important step toward managing its effects and maintaining an active lifestyle. In this post, we’ll explore the different types of shoulder arthritis, their symptoms, diagnostic approaches, and available treatment options.
Key Takeaways
- Shoulder arthritis is a common condition that can cause significant pain and stiffness.
- Several types of arthritis affect the shoulder, including osteoarthritis, rheumatoid arthritis, and posttraumatic arthritis.
- Treatment options range from non-surgical methods, such as physical therapy and medication, to various surgical procedures.
The Shoulder Joint: A Complex Structure
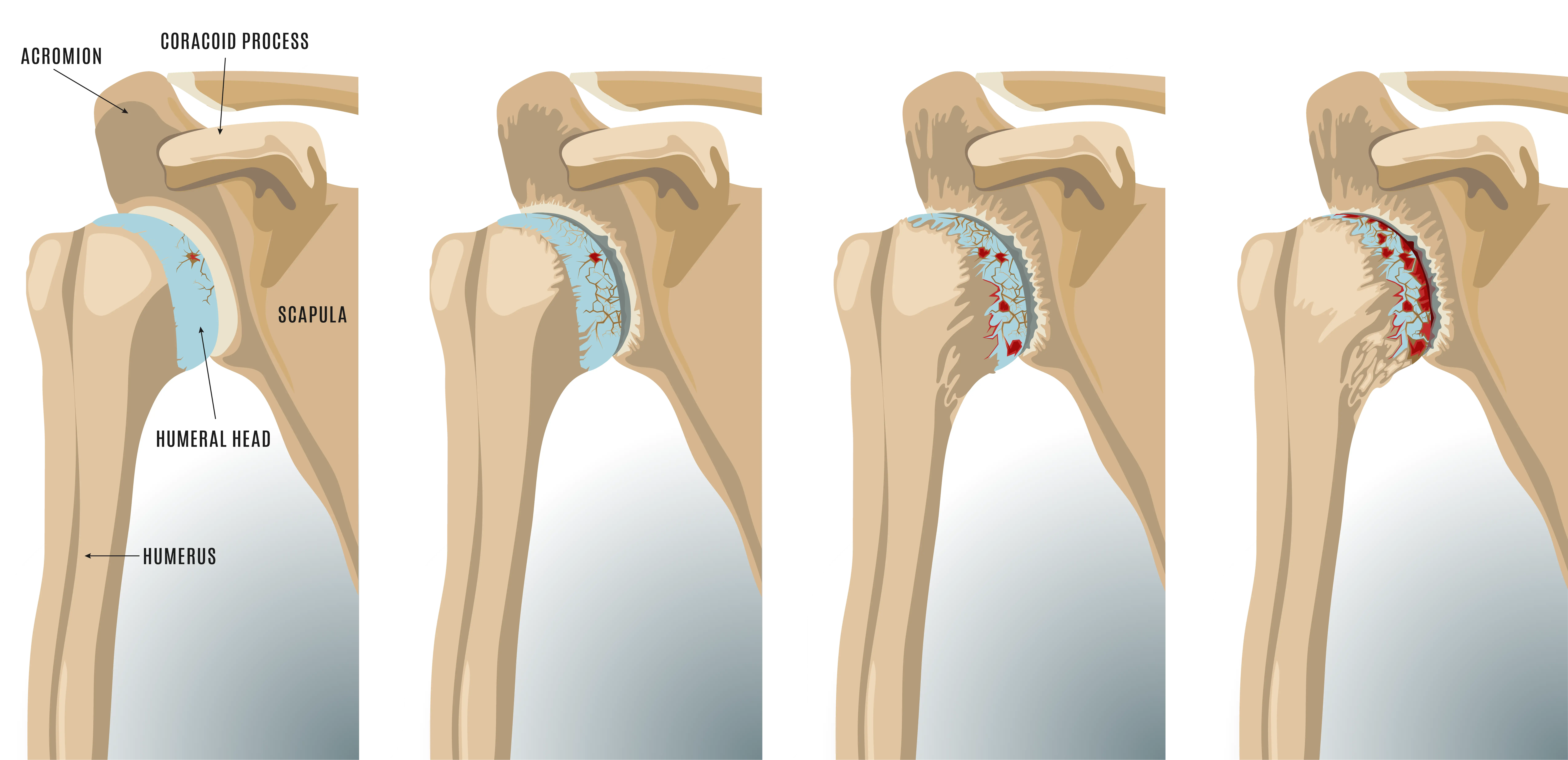
The shoulder joint is composed of three main bones: the humerus, which is your upper arm bone; the scapula, commonly known as your shoulder blade; and the clavicle, or collarbone. These bones form two primary joints within the shoulder complex. The acromioclavicular (AC) joint connects the clavicle to the acromion, a part of the scapula. The glenohumeral joint, often referred to as the main or ball-and-socket shoulder joint, is where the rounded head of the humerus fits into a shallow socket on the scapula called the glenoid.
A smooth, slippery tissue called articular cartilage covers the ends of these bones. This cartilage helps the bones glide effortlessly against each other during movement. It also acts as a shock absorber, protecting the joint from impact. When this cartilage begins to wear away or becomes damaged, the smooth movement of the joint can be compromised, potentially leading to arthritis.

Types of Arthritis Affecting the Shoulder
When people ask, “Can you get arthritis in your shoulder?” they might not realize that several distinct types of arthritis can impact this joint. Each type has its own characteristics, causes, and progression. Recognizing the specific type of arthritis can help guide treatment decisions.
Osteoarthritis (OA)
Osteoarthritis is perhaps the most common form of arthritis, often referred to as “wear-and-tear” arthritis. It commonly affects individuals over the age of 50. In OA, the articular cartilage, which cushions the ends of the bones, gradually breaks down. As this protective cartilage erodes, the bones begin to rub directly against each other. This friction can cause pain, stiffness, and a grinding sensation. Bone spurs, or osteophytes, may also develop around the joint edges.
Rheumatoid Arthritis (RA)
Rheumatoid arthritis is a chronic inflammatory disorder that affects multiple joints throughout the body. Unlike OA, RA is an autoimmune disease. This means the body’s immune system mistakenly attacks its own healthy tissues, specifically the synovium. RA frequently affects joints symmetrically, meaning it might impact both shoulders simultaneously.
Posttraumatic Arthritis
As its name suggests, posttraumatic arthritis develops following a physical injury to the shoulder. Injuries such as fractures, dislocations, or severe sprains can damage the articular cartilage or alter the joint’s mechanics. Even after the initial injury heals, the altered joint surface or ongoing inflammation can accelerate cartilage breakdown. Over time, this can lead to the development of arthritic symptoms.
Rotator Cuff Tear Arthropathy
The rotator cuff is a group of muscles and tendons that surround the shoulder joint, providing stability and enabling arm movement. A large, long-standing tear in one or more of these tendons can lead to a specific type of arthritis known as rotator cuff tear arthropathy. When the rotator cuff is severely damaged, it may no longer effectively hold the head of the humerus in its proper position within the glenoid socket. This instability can allow the humeral head to migrate upward, rubbing against the acromion.
Avascular Necrosis (AVN)
Avascular necrosis, or osteonecrosis, of the shoulder occurs when the blood supply to the head of the humerus is disrupted. Without an adequate blood supply, bone cells begin to die. This process can cause the bone to collapse, leading to damage of the overlying articular cartilage and, eventually, arthritis. Several factors may contribute to AVN, including long-term or high-dose steroid use, heavy alcohol consumption, sickle cell disease, and traumatic injuries like shoulder fractures. In some instances, a clear cause cannot be identified, and the condition is then referred to as idiopathic AVN.
Recognizing the Symptoms of Shoulder Arthritis
Understanding the symptoms of shoulder arthritis is helpful for early detection and effective management. While symptoms can vary depending on the type and severity of arthritis, some indicators may suggest the presence of the condition.
Pain
Pain is a common symptom associated with shoulder arthritis. This pain often worsens with activity and tends to progress over time. If the glenohumeral joint is involved, you might feel a deep ache in the side or back of your shoulder. For arthritis affecting the AC joint, the pain typically localizes to the top of the shoulder. As arthritis advances, nearly any movement of the shoulder can become painful. Many people also report night pain, which can disrupt sleep patterns and impact overall quality of life.
Limited Range of Motion
Shoulder arthritis can restrict your ability to move your arm freely. You might find it increasingly difficult to perform everyday tasks, such as lifting your arm to brush your hair, reaching for objects on a high shelf, or fastening clothing behind your back. This limitation in movement can stem from pain, stiffness, or mechanical blockages within the joint due to cartilage loss and bone spurs.
Crepitus
Crepitus refers to a grinding, clicking, or snapping sensation or sound that occurs when you move your shoulder. This phenomenon results from the rough surfaces of damaged cartilage or bone rubbing against each other. While crepitus is not always painful, it can sometimes be accompanied by discomfort.
Other Potential Symptoms
Individuals with shoulder arthritis might also experience:
- Stiffness: Especially noticeable after periods of inactivity, such as waking up in the morning or after sitting for a long time.
- Tenderness: The joint area may feel tender to the touch.
- Swelling: Although less common in the shoulder than in other joints, some swelling might occur.
- Weakness: Pain and disuse can lead to muscle weakness around the shoulder.
Diagnosing Shoulder Arthritis
Accurate diagnosis is important for developing an effective treatment plan for shoulder arthritis. An experienced shoulder specialist will typically employ a combination of methods to determine the presence and type of arthritis affecting your shoulder.
Medical History and Physical Examination
Your doctor will begin by taking a detailed medical history. They may ask about your symptoms, including when they started, how they have progressed, and what activities aggravate or alleviate your pain. They will also inquire about any previous shoulder injuries, medical conditions, and medications you are taking.
Following the history, a thorough physical examination of your shoulder may be conducted. During this examination, your doctor will assess tenderness, range of motion, stability, crepitus, and pain.
Imaging Tests
Imaging studies can provide visual information about the condition of your shoulder joint. Tests may include:
- X-rays: X-rays create detailed images of dense structures like bone. For an arthritic shoulder, X-rays may reveal several characteristic signs, including a narrowing of the joint space, changes in the bone structure, and the formation of bone spurs (osteophytes).
- Magnetic Resonance Imaging (MRI): An MRI provides more detailed images of soft tissues, including cartilage, tendons, and ligaments. While X-rays are excellent for bone, MRI can better visualize the extent of cartilage damage, inflammation, and rotator cuff tears.
- Computed Tomography (CT) Scan: A CT scan offers cross-sectional images of the bone, providing a more detailed view of bone structure and any deformities. This can be particularly useful in planning surgical interventions.
Treatment Options for Shoulder Arthritis
Treatment strategies aim to reduce pain, improve function, and slow the progression of joint damage. Both non-surgical and surgical options may be available depending on your condition.
Non-Surgical Treatments
Non-surgical approaches can be effective in managing symptoms for many individuals.
- Activity Modification: Adjusting daily activities to avoid movements that aggravate your shoulder pain can make a difference. This might involve modifying exercise routines, changing work habits, or using assistive devices. Learning to move your arm in ways that minimize stress on the joint is a practical strategy.
- Physical Therapy: A structured physical therapy program is typically a cornerstone of non-surgical management. A physical therapist can teach you exercises to strengthen the muscles around your shoulder, improve flexibility, and restore range of motion.
- Medications:
- Nonsteroidal Anti-inflammatory Drugs (NSAIDs): Over-the-counter NSAIDs, such as ibuprofen or naproxen, may be used to help reduce pain and inflammation.Corticosteroid Injections: These injections deliver an anti-inflammatory medication directly into the shoulder joint. Corticosteroids can provide significant, though often temporary, pain relief and reduce inflammation.
- Disease-Modifying Antirheumatic Drugs (DMARDs): For inflammatory types of arthritis, such as rheumatoid arthritis, specific medications to suppress the immune system may be prescribed.
- Heat and Ice: Applying moist heat can help relax stiff muscles and increase blood flow to the area, while ice packs can reduce inflammation and numb pain. Many people find alternating between heat and ice beneficial for symptom relief.
Surgical Treatments
When non-surgical treatments no longer provide adequate relief, or if the arthritis is severely impacting your quality of life, surgical intervention might become a viable option. Several surgical procedures may be used to address shoulder arthritis, each suited to different conditions and patient needs.
- Arthroscopy: For milder cases of shoulder arthritis, arthroscopy may be an option. This minimally invasive procedure involves making small incisions and inserting a tiny camera (arthroscope) into the joint. The surgeon can then use small instruments to remove loose pieces of cartilage, clean out inflamed tissue, or shave down bone spurs. Arthroscopy can help relieve pain and improve function, though it may not stop the progression of arthritis.
- Shoulder Joint Replacement (Arthroplasty): The goal of shoulder replacement surgery is to relieve pain and restore movement by replacing the damaged parts of the joint with artificial components, known as prostheses. There are several types of shoulder replacement:
- Total Shoulder Arthroplasty: This involves replacing both the head of the humerus with a metal ball and the glenoid socket with a plastic cup. Total shoulder arthroplasty is a common treatment option for severe glenohumeral osteoarthritis.
- Reverse Total Shoulder Arthroplasty: This specialized procedure is often recommended for individuals with rotator cuff tear arthropathy or those with severe arthritis and a non-functional rotator cuff. In a reverse total shoulder replacement, the ball and socket components are switched. A metal ball is attached to the scapula where the glenoid used to be, and a plastic cup is attached to the top of the humerus. This design allows the deltoid muscle, rather than the damaged rotator cuff, to power arm movement.
Your surgeon will discuss the most suitable surgical option based on your specific condition, age, activity level, and overall health.
Summary
Shoulder arthritis is a common condition that can impact an individual’s quality of life. It encompasses several distinct types, each with unique causes and characteristics. Knowing the symptoms, such as pain, limited motion, and crepitus, is the first step toward seeking appropriate medical attention. A thorough diagnosis, involving physical examination and imaging, helps pinpoint the specific type and severity of the arthritis. A wide array of treatment options exists, ranging from conservative non-surgical approaches like physical therapy and medication to various surgical interventions, including different types of shoulder replacement.
Frequently Asked Questions (FAQ)
How is shoulder arthritis diagnosed?
Diagnosis typically involves a comprehensive medical history, a physical examination to assess movement and pain, and imaging tests such as X-rays, MRI, or CT scans.
What are the non-surgical treatment options for shoulder arthritis?
Non-surgical treatments may include activity modification, physical therapy, pain medications (like NSAIDs), corticosteroid injections, and applying heat or ice. For inflammatory arthritis, specific disease-modifying drugs may be prescribed.
When is surgery recommended for shoulder arthritis?
Surgery is generally considered when non-surgical treatments no longer provide sufficient pain relief or when the arthritis severely limits daily activities. Surgical options range from arthroscopy to various types of shoulder replacement.





